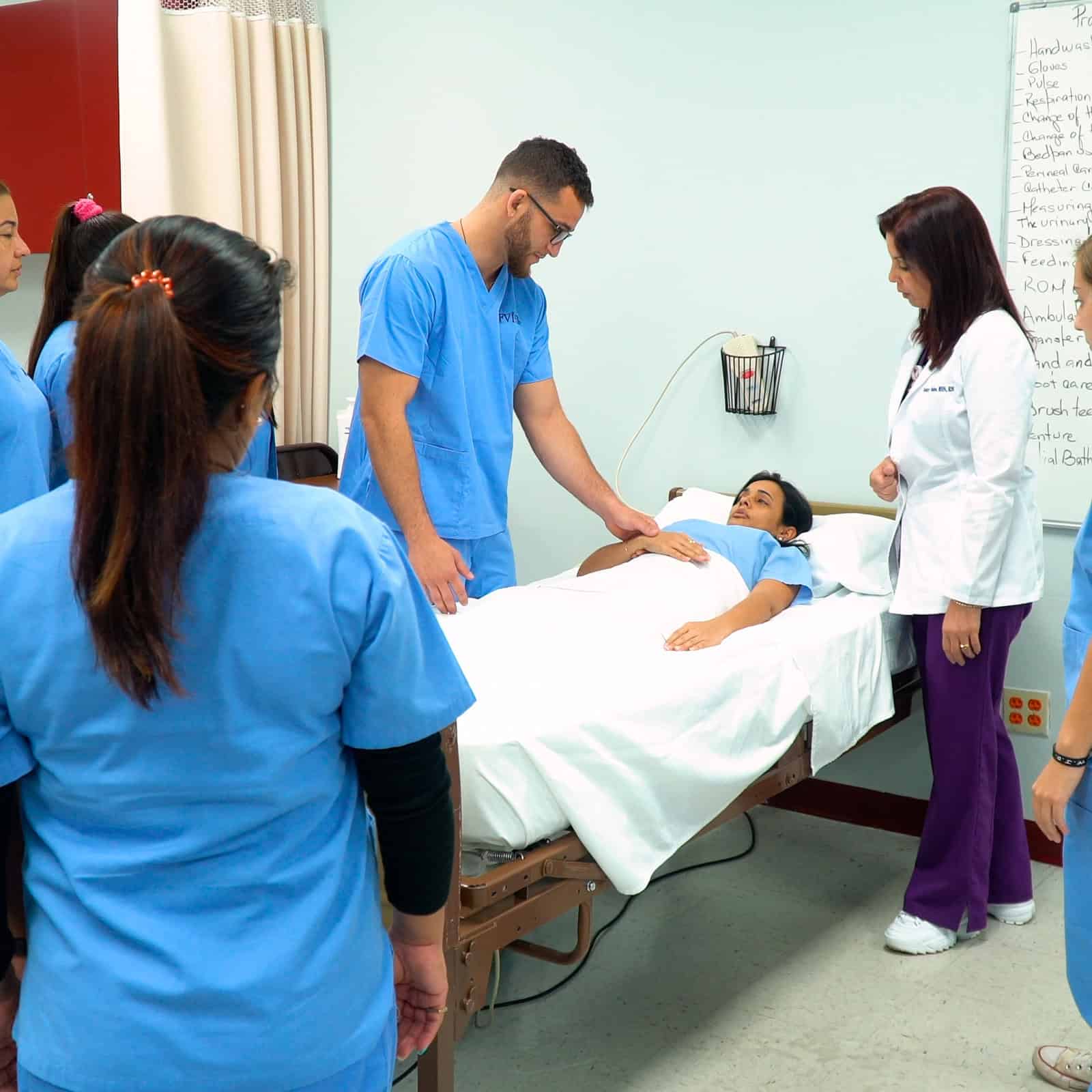
Will Hospitals Hire Nurses with ASNs in Miami?
Yes, hospitals in Miami do hire nurses with an Associate of Science in Nursing (ASN) degree. An ASN is the[...]

How Foreign-Trained Doctors Can Pursue Nursing Careers in South Florida: Your Path to RN Licensure
Foreign-trained physicians in South Florida sometimes choose to pursue a nursing career as a streamlined way to enter the U.S.[...]

How To Become a Nurse in Little Havana, FL
Little Havana is a vibrant Miami neighborhood with a strong Cuban heritage, where many families stay closely connected across generations.[...]

How To Become a Nurse in Sunset, FL
Sunset, FL, is a welcoming suburban neighborhood in Miami-Dade County, home to thriving Cuban, Colombian, and Haitian communities that each[...]

Growing Demand for Bilingual Spanish-Speaking Nurses in Miami’s Healthcare System
Miami is one of the most Hispanic-majority cities in the U.S., and the Hispanic/Latino community makes up 70% of Miami-Dade[...]

Pursuing a Nursing Career in Miramar, FL: A Guide for Haitian Students
Miramar, FL, has a large and growing Haitian community, high demand for Creole-speaking nurses, and close proximity to hospitals and[...]

How To Become a Nurse in Westchester, FL
Westchester, FL, is a well-established Miami-Dade community with a strong Hispanic identity and a very significant Cuban and Cuban-American presence.[...]

How To Become a Nurse in Kendall, FL
Kendall, FL, is a well-established community within Miami-Dade County, shaped by strong family ties and a rich mix of Hispanic,[...]